Objective: To quantify the acute impact of the February 28, 2026 geopolitical escalation on population-level sleep health using continuous wearable monitoring, in the context of broader implications for mental health surveillance and proactive intervention.
Data: ~5.4 million user-days from ~180,000 daily active Ultrahuman Ring AIR users across 46 countries (February 1–March 1, 2026). March 1 values compared against a 27-day pre-escalation baseline; cross-country changes evaluated using normalized relative disruption metrics and time-series trajectories.
Findings:
Conclusion: Sleep disruptions concentrated in Gulf nations and were detectable on the same night as the escalation. These findings underscore the link between geopolitical stress and physiological health, and suggest continuous wearable monitoring could serve as a real-time early warning system for mental health, not just at individual level but also at population-level.
Major geopolitical events are conventionally evaluated through military, diplomatic, and economic frameworks. Less visible, yet arguably no less consequential, is their physiological toll on civilian populations, including individuals geographically remote from active conflict. Sleep is among the most sensitive biomarkers of psychological stress.¹⁻³
Acute psychological distress activates the hypothalamic-pituitary-adrenal (HPA) axis and the sympathetic nervous system, producing hyperarousal that disrupts sleep continuity and REM architecture, both critical for emotional regulation and cognitive recovery.³ REM sleep is essential for processing emotions and consolidating memories; its suppression under acute stress is one mechanism by which external events can translate into mental health vulnerability.
Sleep disruption is not merely a symptom of stress; it is a recognized driver of downstream mental health deterioration. Stress breaks sleep, and broken sleep amplifies stress, accelerating the progression toward anxiety and depression.⁴˒⁵ Population-level sleep disturbance during geopolitical crises may therefore represent an early, measurable signal of emerging mental health burden, one that precedes clinical presentation and is amenable to early intervention.
Wearable devices have enabled continuous, real-time measurement of sleep at population scale, providing an objective means to detect biological disruption during external crises, including armed conflict,⁶ pandemic lockdowns,⁷ and major political events,⁸ without requiring self-report during already stressful periods.
This study leverages continuous Ultrahuman Ring AIR sleep data from ~180,000 daily active users across 46 countries, representing 5.4 million user-days, to examine how sleep patterns changed during a major geopolitical escalation. By comparing each country's sleep metrics against its own recent baseline and tracking daily changes over time, we assess how disruption varied across regions and consider how these patterns inform the need for scalable, technology-enabled mental health support.
We analyzed aggregate, de-identified data from approximately 180,000 daily active Ultrahuman Ring AIR users across 46 countries between February 1 and March 1, 2026, representing approximately 5.4 million user-days of continuous monitoring. Four Gulf countries (the United Arab Emirates, Qatar, Saudi Arabia, and Kuwait) were examined as the primary exposure group due to their geographic and geopolitical proximity to the February 28 escalation. Daily national averages were computed for multiple sleep metrics: sleep score, sleep efficiency, awake time, REM sleep percentage, deep sleep percentage, and total sleep time.
March 1 values were compared against a 27-day pre-escalation baseline (February 1–27). Absolute changes were calculated as the difference between the March 1 value and the country-specific baseline mean. To enable cross-country comparability, deviations were standardized relative to baseline variability and subsequently normalized per metric by dividing each country's absolute change by the maximum absolute change observed across all 46 countries. This yielded a relative disruption scale ranging from −1 to +1, where −1 denotes the largest observed disruptive deviation for a given metric.
For awake time, the sign convention was inverted so that increases (indicative of greater disruption) aligned directionally with declines in other sleep metrics. Temporal dynamics were assessed by plotting daily national averages from February 1 through March 1.
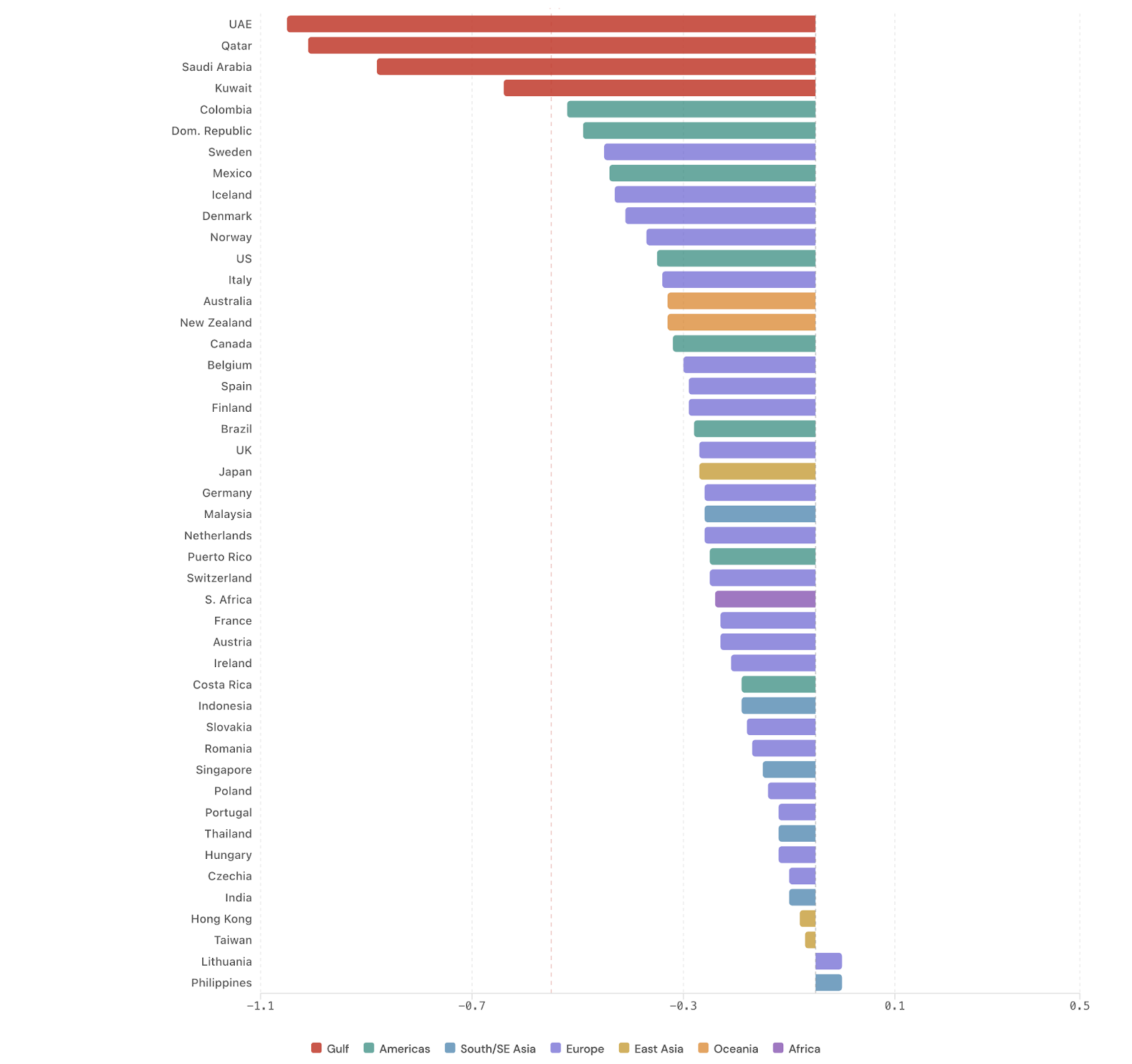
A clear geographic gradient was evident on March 1 (Figure 1A). Gulf countries occupied the most extreme positions in the cross-country ranking, with the UAE exhibiting the largest relative decline in sleep score (−1.00), followed by Qatar (−0.96), Saudi Arabia (−0.83), and Kuwait (−0.59). Countries outside the Gulf demonstrated substantially smaller deviations, with most clustering between −0.30 and −0.05.
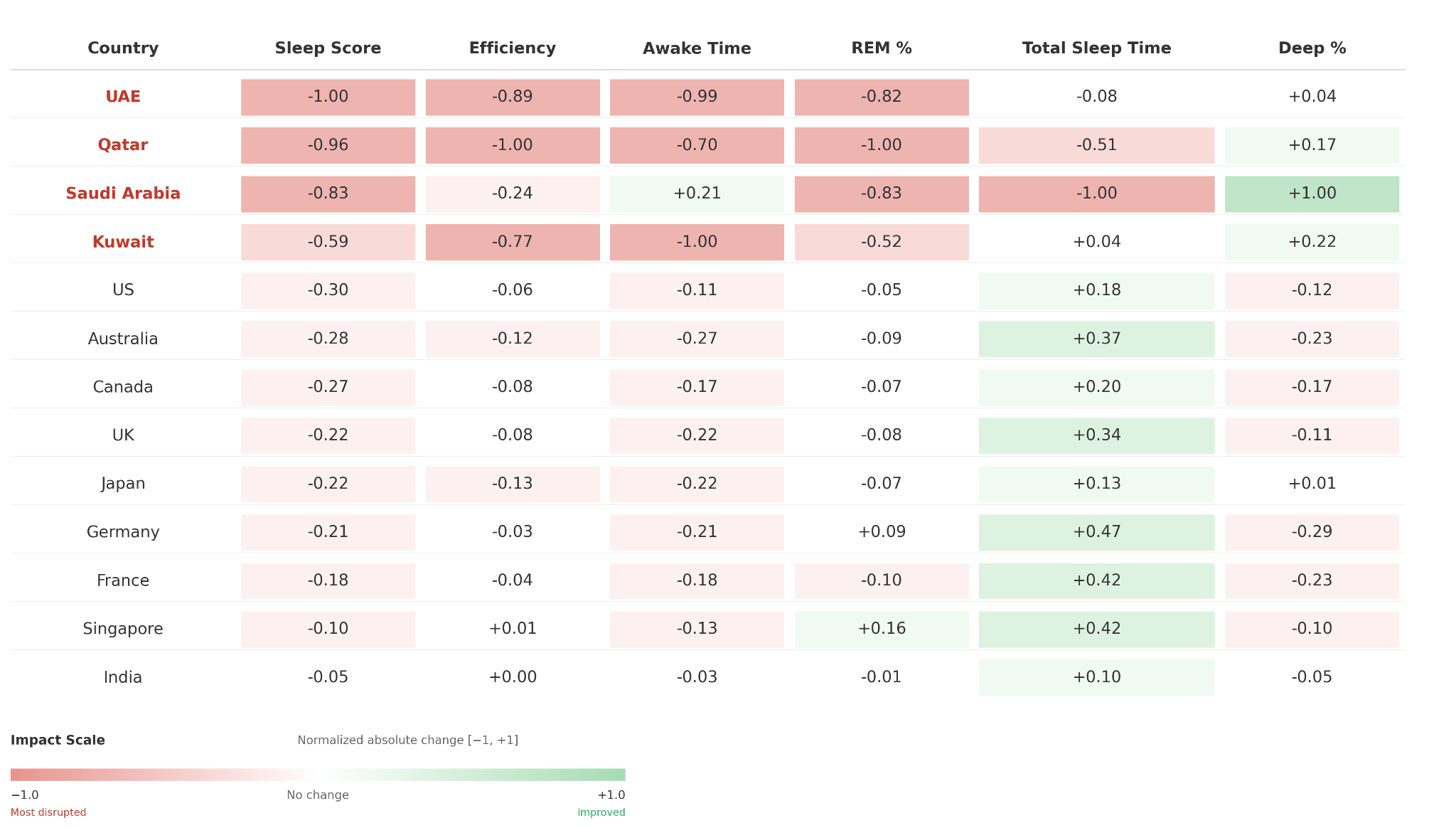
The per-metric comparison reinforces this pattern (Figure 1B). The UAE (2,878 users) recorded the maximum decline in sleep score (−1.00) with near-maximal disruption in sleep efficiency (−0.89), awake time (−0.99), REM sleep (−0.82), alongside smaller change in total sleep duration (−0.08). Qatar (381 users) showed the greatest decline in sleep efficiency (−1.00) and REM sleep (−1.00), alongside a sleep score reduction of −0.96 and a notable reduction in total sleep duration (−0.51). Kuwait (208 users) showed maximum disruption in awake time (−1.00) despite a moderate sleep score (−0.59), suggesting a distinct pattern of stress expression. Saudi Arabia (971 users) showed considerable reductions in sleep score (−0.83), REM sleep (−0.83), and total sleep duration (−1.00), with smaller changes in sleep efficiency (−0.24), while awake time changed in the opposite direction (+0.21).
In contrast, the United States (71,753 users; −0.30 sleep score), Australia (−0.28), the United Kingdom (11,184 users; −0.22), and India (18,631 users; −0.05) showed modest changes. Sleep disruption was concentrated in Gulf nations rather than distributed uniformly across the global user base.
A)
B)
Time-Series Analysis Reveals Acute Post-Escalation Disruption Superimposed on Gradual Shifts
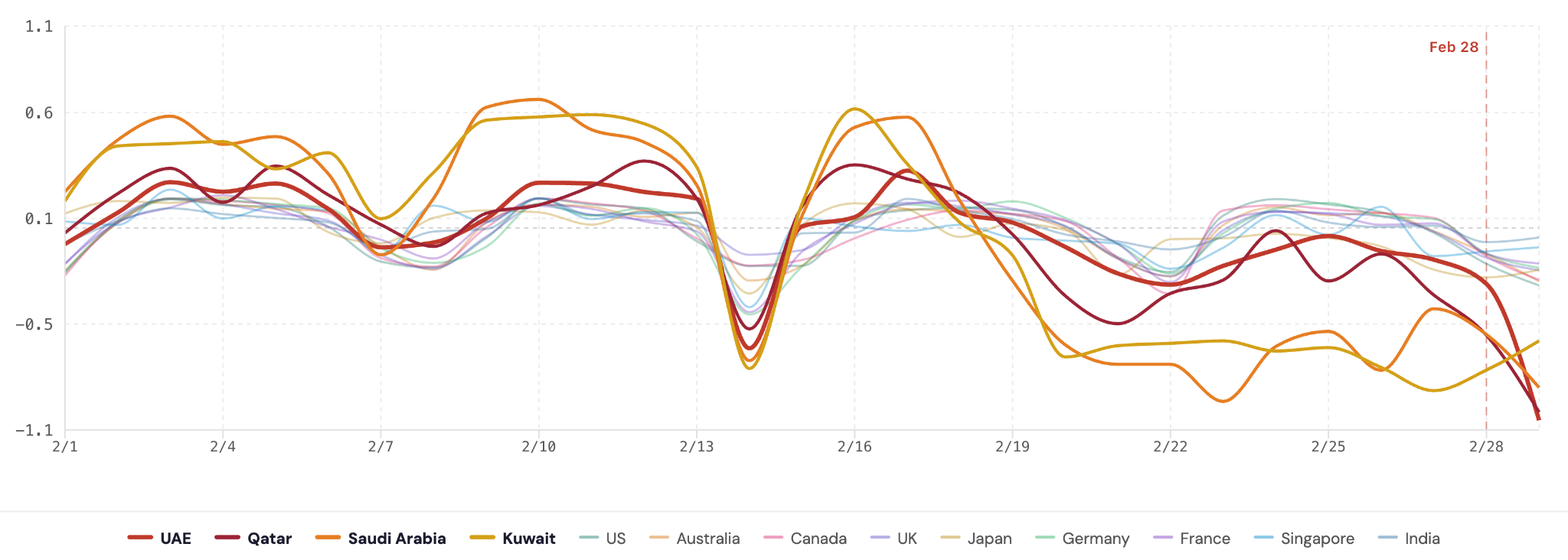
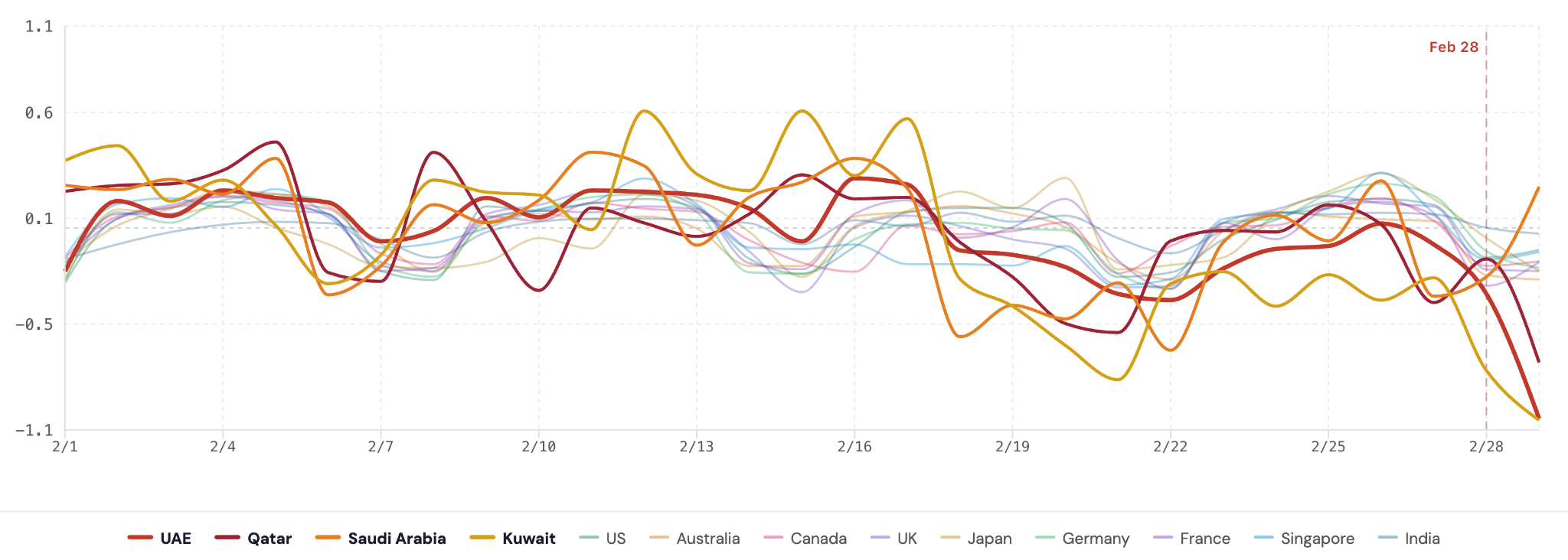
Daily normalized deviations from baseline revealed relative stability across countries during early February (Figures 2A-D), with most values remaining within approximately ±0.20 of baseline prior to February 28.
A transient dip around February 13-14 was observed across several countries in sleep score and sleep efficiency, with deviations generally ranging between −0.30 and −0.50 in affected nations. This period coincided with multiple concurrent influences, including a widely observed mid-February holiday, weekend-related behavioral shifts, and escalating geopolitical tensions. The magnitude of this deviation appears moderate relative to the subsequent event-related shifts.
Beginning February 19, progressive divergence was observable in select Gulf countries, particularly Saudi Arabia and Kuwait, where sleep score and awake time deviations gradually approached −0.50 to −0.70. This interval overlaps with the commencement of Ramadan in 2026, a period established to alter sleep timing and consolidation.⁹˒¹⁰ The gradual rather than abrupt character of these shifts is consistent with volitional, culturally driven behavioral schedule modifications.
Following this phase, February 28 was marked by a sharp, concentrated drop across multiple metrics in Gulf countries. Sleep score and efficiency rapidly approached −0.90 to −1.00 in the UAE and Qatar, while awake time and REM sleep moved toward maximal disruption. Comparison countries remained closer to baseline, typically within −0.30.
Taken together, the time-series data show that February 28 is associated with a simultaneous shift across Gulf countries that is distinct in both magnitude and abruptness from the gradual Ramadan-related shifts and the transient mid-February dip.
A) Sleep Score
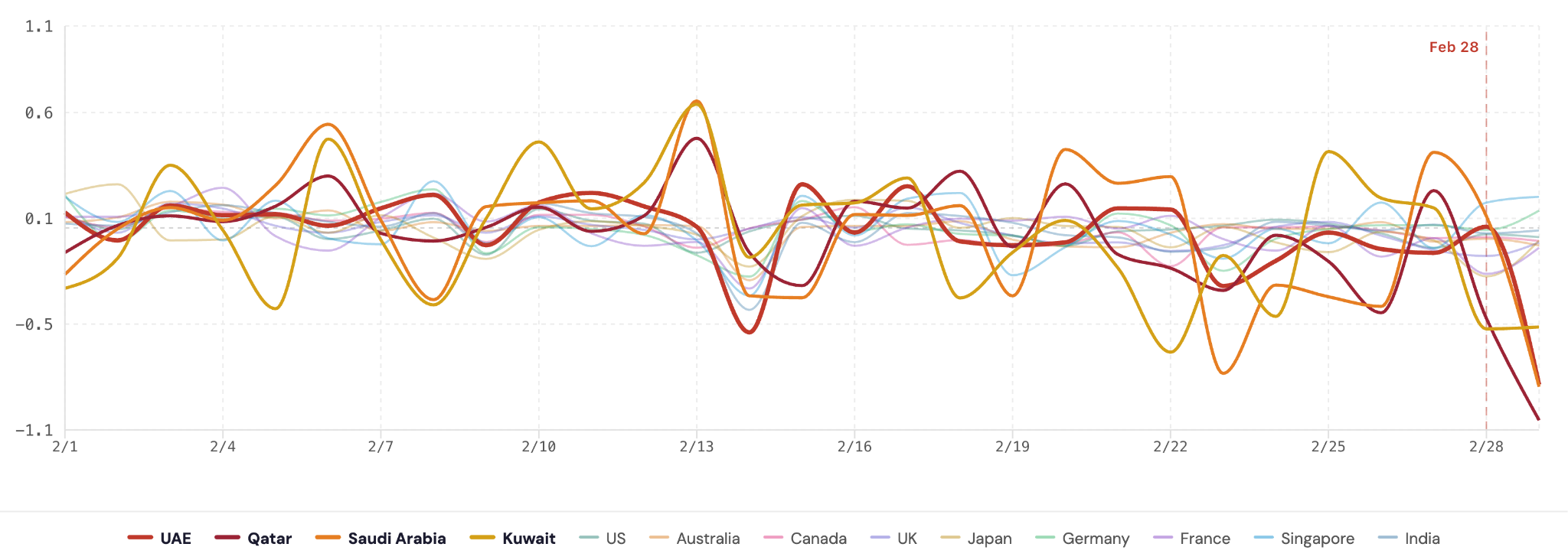
B) Sleep Efficiency
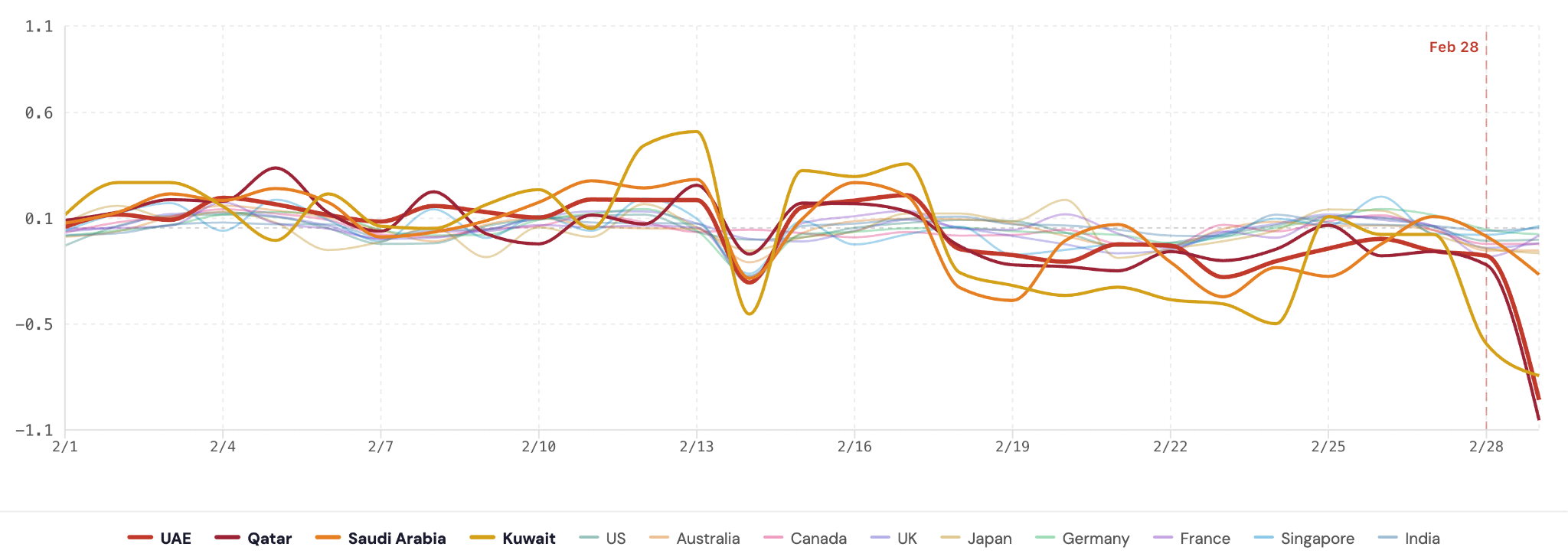
C) Time Spent Awake
D) REM Sleep Percentage
The February 28 geopolitical escalation was associated with sharp, simultaneous declines in sleep score, efficiency, awake time, and REM sleep across Gulf nations. The geographic gradient, most severe in the UAE and Qatar, moderate in Saudi Arabia and Kuwait, mild elsewhere, is consistent with evidence that populations closer to conflict bear a greater physiological and psychological burden.¹¹ These shifts were detectable through wearable data on the same night, without requiring self-report.
The pattern is consistent with established stress–sleep neurobiology: acute psychological stress activates the HPA axis and sympathetic nervous system, producing hyperarousal that fragments sleep and suppresses REM.²˒³ REM sleep is essential for emotional regulation and memory consolidation; its suppression is one pathway by which external events can translate into personal mental health vulnerability. Deep sleep, by contrast, remained largely unchanged, which is consistent with prior findings that slow-wave sleep may be relatively preserved under acute psychological stress compared to lighter sleep stages and REM.¹˒³
While most metrics showed directionally consistent declines, each Gulf nation exhibited a distinct pattern of disruption, suggesting that more granular, individualized assessment may be important for understanding and responding to stress-related physiological changes.
Sleep disturbance is both a symptom of and risk factor for anxiety, depression, and PTSD.⁴˒⁵ When stress disrupts sleep, broken sleep can amplify the stress response, creating a reinforcing cycle that accelerates progression toward psychiatric conditions.¹˒² Populations exposed to geopolitical instability show elevated rates of insomnia and psychological distress,¹¹ and the depth of disruption observed here across multiple sleep dimensions suggests a physiological burden that self-report measures alone may not capture. Population-level sleep disruption during periods of conflict may therefore reflect emerging psychological strain before it becomes clinically apparent.
Continuous wearable monitoring makes it possible to detect the biological signatures of psychological stress as they emerge. As demonstrated in this study, large external events can produce measurable disruptions in sleep architecture across entire populations, often before individuals consciously recognize distress. Wearable sleep data therefore provide an objective window into collective physiological responses, revealing how the body registers external uncertainty in real time. Identifying these changes early may help inform timely awareness, supportive resources, and preventive interventions. At population scale, wearable monitoring offers a means of recognizing emerging mental health burden earlier and responding more proactively during periods of societal stress.